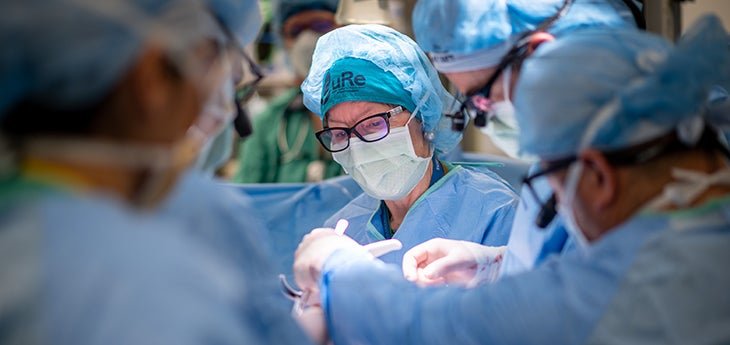
Michelle Johnson was 20 weeks into her pregnancy when she learned her unborn son had spina bifida. Because his spine hadn’t fully sealed, the spinal cord was left protruding from a gaping hole. Without surgery, he would face a lifetime of disabilities.
So she jumped at the prospect to enroll in a small experimental trial for the condition on the University of California, Davis. The treatment combines fetal surgery, an existing approach, with a dose of stem cells to spur healing.
Now 4 years old, Johnson’s son Tobi can walk and lacks symptoms equivalent to lack of bladder and bowel control. “Tobi’s physical and mental abilities are nothing in need of a miracle,” she said in a press release.
Tobi is one in every of six children within the CuRe trial, the primary study to check if using stem cells to repair tissue in fetuses with spina bifida is protected. Delivered by a small patch sewn onto the damaged site, the stem cells protected the spinal cord from inflammation and helped the wound heal. Not one of the babies or moms suffered short-term uncomfortable side effects, like unwanted tissue growth or cancer.
With so few participants, it’s too early to inform how the approach will pan out as the youngsters grow. But due to the promising safety profile, the FDA has approved the enrollment of more pregnant women with the identical diagnosis.
“This can be a major step toward a brand new form of fetal therapy, one which doesn’t just repair but potentially helps heal and protect the developing spinal cord,” study writer Aijun Wang said within the press release.
CuRe joins other attempts to tackle diseases with stem cells within the womb. Although a really young field, the approach could slow, halt, or cure quite a lot of diseases before babies are born.
A Head Start
Spina bifida is a condition where the spine or spinal cord doesn’t properly seal during development. One in 2,875 newborns are affected within the US yearly. In its most severe form, cerebrospinal fluid—a liquid that surrounds the brain and washes out toxins—builds up, causing progressive damage to the fetal spinal cord, lifelong movement problems, and even paralysis.
The condition was first treated after birth, when surgeons would close the defect. But by then, the damage was done. Surgery before birth could stave off symptoms, an idea validated in a 2011 trial. Yet over half of treated babies still struggled to walk without help, likely because injured neurons within the fetuses’ brains and spinal cords didn’t have the prospect to heal.
Stem cells spur regrowth by releasing protective nutrients, and the fetal environment is uniquely suited to the cells. The team wondered if adding them could improve prenatal surgery.
They began testing the concept around 2012 using induced pluripotent stem cells. This can be a kind of stem cell constituted of skin or other mature cells using a chemical cocktail. Taking this approach could provide a virtually unlimited supply of stem cells. However it didn’t work.
After years of trial and error, the team found success with stem cells derived from placentas. The cells protected neurons from injury and encouraged their growth in lab dishes. In addition they healed defects in a lamb model of spina bifida. Newborns receiving the cells together with prenatal surgery could arise and walk; those that only had surgery couldn’t.
Stem cell therapy appeared promising. But for unborn babies, it could carry risk. Because the cells come from donors, they could spark immune reactions. They may also trigger abnormal tissue growth, and even cancer. Because stem cell treatments are rarely utilized in the womb, little is thought about their effects on pregnancy or the general health of mother and baby.
Landmark Trial
The primary stage of the CuRe trial focused on these safety concerns.
The team seeded a small patch with stem cells derived from donated placental tissue. To assist the cells integrate, the researchers designed the patch to mimic conditions normally surrounding cells.
Surgeons made a small opening within the uterus at 24 to 25 weeks into pregnancy and gave the fetus a small dose of painkillers and muscle relaxers. They then placed the stem cell patch onto the exposed spinal cord and sutured the gap closed.
The trial closely monitored six babies, including Tobi, for possible uncomfortable side effects. After delivery by C-section, none had complications, equivalent to leaking cerebrospinal fluid, infection, or signs of cancer. In all cases, the treatment prevented parts of the brain from slipping into the neck, and none required a shunt—a small tube used to empty excess fluid from the brain—an encouraging sign of success.
The team turned to stem cells, they wrote, since the cells can lessen brain inflammation and brain cell death. At the identical time, they pump out growth proteins that “support neural tissue preservation and spinal cord integrity.”
The researchers designed the study to judge safety not determine whether stem cells enhance the surgery’s results. But Tobi’s remarkable recovery is a hopeful sign that the cells do make a difference. Because spina bifida is structural, treating it before everlasting damage occurs could make the therapy a “one-and-done” fix.
The study joins the growing prenatal use of stem cells in conditions equivalent to thalassemia, a blood disorder, and osteogenesis imperfecta, also often known as brittle bone disease. Early clinical trials have shown promise, but regulators haven’t yet approved any treatments.
“Putting stem cells right into a growing fetus was a complete unknown. We’re excited to report great safety,” said Diana Farmer, a study writer and lead investigator for the CuRe trial. “It paves the way in which for brand spanking new treatment options for kids with birth defects. The long run is exciting for cell and gene therapy before birth.”
The team is actively recruiting more pregnant women for the trial’s second phase. They’ll track the youngsters’s growth and health as much as age six to evaluate brain and cognitive development, motor skills, and other growth milestones.
If the treatment proves successful, longer monitoring could also be needed. Spina bifida can increase the chance of kidney disease and certain cancers later in life, and it’s unclear if the stem cells could cause problems months or years down the road.
Uncertainties aside, Johnson is glad to be participating within the trial. “We’re perpetually grateful for the numerous health professionals who supported Tobi’s journey and proceed to observe him conquer the world,” she said.